By Rustam Iuldashov
30 years lived experience with chronic migraine | Sources: 27 peer-reviewed references including Cephalalgia, Pain Physician, American Journal of Neuroradiology, Fluids and Barriers of the CNS, Frontiers in Nutrition, Nutrients | Last updated: March 9, 2026
Medical Review: This content is based on peer-reviewed research from Cephalalgia, Pain Physician, American Journal of Neuroradiology, Fluids and Barriers of the CNS, Headache, Family Practice, Journal of Clinical Neuroscience, Nutrients, and Frontiers in Nutrition.
Important Notice: This article is for informational purposes only and does not replace professional medical advice. The author is not a licensed physician or healthcare professional. Always consult your doctor before making changes to your treatment plan.
Key Takeaways
- Dehydration is a trigger, not a cause — it lowers your migraine threshold, especially when stacked with other triggers[1, 4]
- Plain water can backfire — overhydrating without electrolytes dilutes blood sodium and can cause headaches through the exact mechanism you’re trying to avoid[11, 12]
- Three electrolytes matter most: sodium (fluid balance), magnesium (neuronal stability), and potassium (ion channel function)[9, 14, 17]
- Magnesium deficiency is common in migraineurs but often missed by standard blood tests — oral supplementation (600 mg citrate) has meta-analytic support for prevention[15, 16]
- You can make a hospital-grade rehydration solution at home: water + salt + sugar + lemon[23]
- Light straw-yellow urine — not clear — is the hydration sweet spot[21]
You did everything right. Eight glasses. A bottle on the desk. Another by the bed. And yet the migraine came — the pressure behind the eye, the nausea, the light turning hostile.
Here’s what nobody told you: hydration isn’t about volume. It’s about what your brain does with the water once it arrives. And for a migraine brain, that equation has a very different answer than “just drink more.”
The One-Third Problem
One in three people with migraine identify dehydration as a trigger.[1] The American Migraine Foundation calls even mild dehydration a fast track to debilitating head pain.[2] But “Dehydration Headache” doesn’t exist as a diagnosis. It’s not recognized in the International Classification of Headache Disorders, 3rd edition.[3] Dehydration is a trigger — not a cause. That distinction changes everything.
Think of your migraine threshold as a bucket. Stress fills it a little. Poor sleep adds more. A skipped meal, a little more. Dehydration doesn’t need to overflow the bucket on its own — it just adds to whatever is already inside.[4] On a calm, well-rested day, mild dehydration might not matter. Stack it with two other triggers, and the bucket tips.
What Your Brain Actually Needs
Your brain is roughly 75% water. Every electrical signal it sends depends on precise fluid balance.[5] Lose just 1–2% of your body’s fluid, and the machinery starts to strain.
How much strain? An MRI study of 15 healthy individuals showed that 12 hours without water reduced brain tissue fluid by 1.6%, with measurable shrinkage in cortical thickness, white matter volume, and overall brain size.[6] The changes reversed within an hour of rehydration. But until they did, those brains were operating in a compromised state — thinner, tighter, less resilient.
The mechanism isn’t fully mapped. Researchers at Migraine Canada point to the brain’s osmolarity — the concentration of dissolved particles in the fluid surrounding neurons.[7] When that fluid becomes too concentrated, certain pain receptors may activate and trigger an attack. Your brain doesn’t just need water. It needs the right ratio of water to electrically charged minerals — electrolytes — to keep its signaling stable.[8]
Water without electrolytes is like fuel without a spark plug. Necessary, but insufficient.
The Electrolyte Cast: Sodium, Magnesium, Potassium
Three minerals run the show. Each plays a distinct role in whether your migraine threshold holds or collapses. Magnesium is the silent guardian. A systematic review confirms that deficiency is linked to abnormal neurotransmitter release, but oral magnesium significantly reduced attack frequency in trials.[14, 16]
Sodium is the lead actor. Researchers at Huntington Medical Research Institutes discovered that cerebrospinal fluid sodium rises during migraine attacks — independently of blood sodium, and independently of every other measured electrolyte in the spinal fluid.[9] A follow-up study revealed something remarkable: CSF sodium follows a 12-hour rhythm, peaking at 8:00 AM and 6:10 PM.[10] Those are exactly the windows when migraine attacks most commonly begin. Correlation, not proof — but the coincidence demands attention.
Now the paradox. Both too little and too much sodium trigger headaches. Drink large amounts of plain water without replacing electrolytes, and you dilute blood sodium — a condition called hyponatremia.[11] The first symptom is headache. When sodium drops too low, fluid rushes into brain cells, swelling them, increasing intracranial pressure.[12] The “just drink more water” advice can create the very problem it claims to solve.
Standard blood tests often miss magnesium issues. Only 1–2% of your body’s magnesium lives in blood serum. Intracellular levels can be dangerously low while your lab results say “normal.”[15]
The evidence for supplementation is real. A meta-analysis of 21 randomized controlled trials — 1,737 participants total — found that oral magnesium significantly reduced both the frequency and intensity of migraine attacks.[16] Not a cure. But a meaningful, low-risk shift in the equation.
Potassium is the newcomer. A 2025 study found that patients with chronic migraine had significantly lower serum potassium (3.76 vs 4.03 mmol/L) and a tenfold higher rate of hypokalemia compared to healthy controls.[17] Population-level data from over 10,000 US adults linked higher dietary potassium to lower odds of severe headache, with an inflection point around 1,439 mg per day.[18] The research is younger and more correlational — but it adds another variable to an equation most people didn’t know existed.
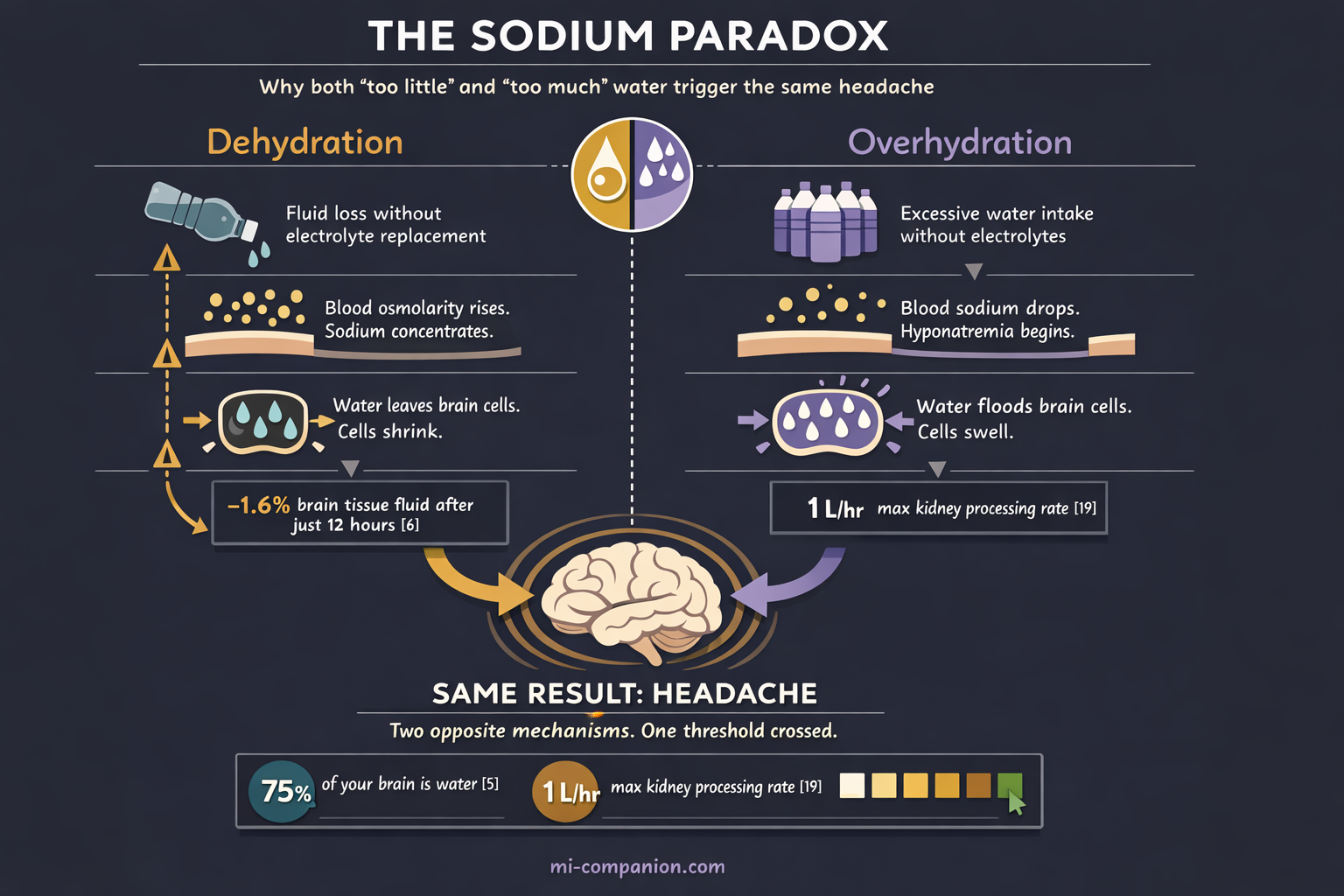
The Overhydration Trap
I’ve lived with migraine for 30 years. For much of that time, “drink more water” was the most common advice I received. So I did — sometimes aggressively. What I didn’t understand is that flooding your body with plain water can backfire spectacularly.
Your kidneys can process about one liter of fluid per hour.[19] Exceed that — or drink heavily while sweating out electrolytes during exercise — and you risk dilutional hyponatremia. The early symptoms are headache, nausea, and brain fog.[20] They mimic dehydration perfectly, creating a vicious loop: you feel bad, you drink more, you feel worse.
Here’s a sign most people read backwards: crystal-clear urine all day long may signal over-dilution, not optimal hydration.[21] The real sweet spot? Light straw yellow. Not clear. Not dark. The color of weak lemonade.
The Practical Equation
⚠️ When to Seek Emergency Help
Severe dehydration with confusion, rapid heartbeat, very dark urine, or inability to keep fluids down requires immediate medical attention. A sudden “worst headache of your life,” new neurological symptoms, or a headache that feels fundamentally different from your usual migraine demands emergency evaluation.
Do not use this article to self-diagnose.
Smart hydration for a migraine brain comes down to rhythm, balance, and awareness. Morning hydration is especially critical, as this is when cerebrospinal fluid sodium peaks and your threshold is most vulnerable.[10]
Rhythm. Sip consistently — roughly one glass every two hours during waking hours — rather than gulping large volumes at once.[22] Steady input keeps osmolarity stable. Large boluses overwhelm the system.
Balance. When you’re sweating, exercising, feverish, or vomiting during a migraine attack, plain water isn’t enough. Adding electrolytes — even a pinch of salt and a squeeze of lemon — activates the sodium-glucose cotransport system that speeds absorption. It’s the same principle behind the WHO oral rehydration formula that has been saving lives in hospitals for decades.[23]
Awareness. For magnesium, international guidelines now recommend 600 mg of magnesium citrate daily as a well-tolerated option for migraine prevention.[24] For potassium, whole foods outperform supplements: bananas, avocados, sweet potatoes, spinach, yogurt.[25]
Your Kitchen Pharmacy: Three Migraine Hydration Formulas
You don’t need expensive powders. The most effective rehydration formula in the world was designed by the WHO using four ingredients you already have.
The Classic ORS (Oral Rehydration Solution)
Based on the same glucose-sodium cotransport principle used in hospitals worldwide.[23] Mix in a large glass or bottle:
- 1 liter of water (room temperature — cold water can trigger nausea during an attack)
- ½ teaspoon of table salt (about 2.5 g — provides ~1,000 mg sodium)
- 6 teaspoons of sugar or honey (about 30 g — the glucose is not optional; it’s the molecular key that unlocks sodium absorption)
- Juice of ½ lemon (adds potassium + makes it drinkable)
Sip slowly over 1–2 hours. Do not gulp. During a migraine attack with nausea, take small sips every 5 minutes rather than large drinks.
The Migraine Morning Tonic
For daily prevention — not during an attack. A lighter formula for the first glass of your day, when CSF sodium peaks and your threshold is most vulnerable:[10]
- 1 tall glass of water (350–400 ml)
- Pinch of sea salt (about ⅛ teaspoon)
- Juice of ¼ lemon
- 1 teaspoon of honey
Drink within 30 minutes of waking, before coffee. Think of it as priming the electrical system before you ask it to work.
The 30-Second Emergency Fix
No lemon? No time? During prodrome or early attack:
- A glass of water + 2–3 small bites of a banana + a few salted crackers or pretzels.
Sodium from the crackers. Potassium from the banana. Water to carry both. It’s not elegant, but it covers all three electrolytes in under a minute.

The Evidence
The numbers back all of this up. A cross-sectional study of 256 women with migraine found significant negative correlations between water intake and every measured migraine characteristic — disability, pain severity, frequency, and duration.[26] An RCT of 102 headache patients found that adding 1.5 liters of water daily for three months improved migraine quality of life scores, with 47% reporting substantial improvement versus 25% in controls.[27]
These aren’t miracle cures. They’re low-risk, low-cost adjustments to a modifiable trigger — the kind of intervention that costs nothing and demands only attention.
Your water bottle isn’t wrong. It’s just incomplete. The equation was never water alone. It’s water plus the minerals that tell your brain what to do with it.
⚕️ Important Medical Disclaimer
This article is for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. The author, Rustam Iuldashov, is not a licensed physician, neurologist, or healthcare professional. He is a patient advocate with 30 years of personal experience living with chronic migraine.
All clinical claims in this article are sourced from peer-reviewed research published in indexed medical journals. Study designs and sample sizes are noted where applicable.
Always consult a qualified healthcare provider for questions about your individual health, migraine treatment, or medication decisions. The information in this article should not replace professional guidance, particularly regarding electrolyte supplementation, magnesium dosing, or any changes to your hydration routine during active medical treatment.
The homemade ORS recipes provided are based on WHO guidelines for general rehydration and are not specifically validated for migraine treatment. This content was last reviewed for accuracy on March 9, 2026.
References
- American Migraine Foundation. “Dehydration and Migraine.” AmericanMigraineFoundation.org (2021). Source: Clinical guideline / Expert consensus.
- American Migraine Foundation, cited in Maharaj N. “Signs of Dehydration That May Lead to a Migraine Attack.” BezzyMigraine (2024). Source: Patient advocacy organization.
- Headache Classification Committee of the International Headache Society. “The International Classification of Headache Disorders, 3rd edition.” Cephalalgia, 38:1–211 (2018). doi:10.1177/0333102417738202. Classification system.
- Pavlovic JM, Buse DC, Sollars CM, Haut S, Lipton RB. “Trigger factors and premonitory features of migraine attacks: summary of studies.” Headache, 54:1670–1679 (2014). doi:10.1111/head.12468. Study design: Systematic review. n=multiple studies.
- Mitchell RH, et al. Neuroscience consensus: brain water composition. Referenced in Ubie Health (2026).
- Biller A, Reuter M, Patenaude B, et al. “Responses of the Human Brain to Mild Dehydration and Rehydration Explored In Vivo by 1H-MR Imaging and Spectroscopy.” American Journal of Neuroradiology, 36:2277–2284 (2015). doi:10.3174/ajnr.A4508. Study design: Prospective cohort. n=15.
- Migraine Canada. “Hydration and Migraine.” MigraineCanada.org (2025). Expert consensus / Educational resource.
- Delgado-López PD, Fernández-de-las-Peñas C, Palacios-Ceña M. “Sodium in Migraine: New Insights into an Old Story.” Cephalalgia, 41(6):759–768 (2021). doi:10.1177/0333102421997280. Study design: Narrative review.
- Harrington MG, Fonteh AN, Cowan RP, et al. “Cerebrospinal fluid sodium increases in migraine.” Headache, 46:1128–1135 (2006). doi:10.1111/j.1526-4610.2006.00445.x. Study design: Prospective cohort. n=31 (20 migraineurs, 11 controls).
- Harrington MG, et al. “Cerebrospinal fluid sodium rhythms.” Fluids and Barriers of the CNS, 7:3 (2010). doi:10.1186/1743-8454-7-3. Study design: Prospective cohort. n=6.
- Cleveland Clinic. “Hyponatremia: Causes, Symptoms, Diagnosis & Treatment.” ClevelandClinic.org (2025). Clinical educational resource.
- StatPearls. “Water Toxicity.” NCBI Bookshelf (2023). Clinical reference / Expert consensus.
- Dominguez LJ, Veronese N, Barbagallo M. “Magnesium and the Hallmarks of Aging.” Nutrients, 16:496 (2024). doi:10.3390/nu16040496. Study design: Narrative review.
- Dominguez LJ, Veronese N, Barbagallo M. “Magnesium and Migraine.” Nutrients, 17(4):725 (2025). doi:10.3390/nu17040725. Study design: Systematic review (PubMed inception to December 2024).
- Maier JA, Pickering G, Giacomoni E, Cazzaniga A, Pellegrino P. “Headaches and magnesium: mechanisms, bioavailability, therapeutic efficacy and potential advantage of magnesium pidolate.” Nutrients, 12(9):2660 (2020). doi:10.3390/nu12092660. Study design: Narrative review.
- Chiu HY, Yeh TH, Huang YC, Chen PY. “Effects of Intravenous and Oral Magnesium on Reducing Migraine: A Meta-analysis of Randomized Controlled Trials.” Pain Physician, 19:E97–E112 (2016). doi:10.36076/ppj/2016.19.E97. Study design: Meta-analysis of 21 RCTs. n=1,737.
- Li X, et al. “Hypokalemia in chronic migraine with medication overuse headache: a retrospective cross-sectional study.” Journal of Headache and Pain, 26 (2025). doi:10.1186/s10194-025-01988-z. Study design: Cross-sectional. n=278 (139+139).
- Xu L, Zhang C, Liu Y, et al. “Association between dietary potassium intake and severe headache or migraine in US adults: a population-based analysis.” Frontiers in Nutrition, 10:1255468 (2023). doi:10.3389/fnut.2023.1255468. Study design: Cross-sectional (NHANES). n=10,254.
- Cleveland Clinic. “Water Intoxication: Toxicity, Symptoms & Treatment.” ClevelandClinic.org (2024). Clinical educational resource.
- Healthline. “Overhydration: Types, Symptoms, and Treatments.” Healthline.com (2023). Health educational resource.
- Ubie Health. “The Salt Secret: How Electrolytes and Hydration Impact Your Migraine Threshold.” UbieHealth.com (2026). Clinical expert review.
- Migraine Canada. “Hydration and Migraine.” MigraineCanada.org (2025). Expert consensus.
- World Health Organization. Oral Rehydration Salts (ORS) formula. WHO clinical guidelines. Referenced in AZ IV Medics (2025).
- von Luckner A, Riederer F. “Magnesium in Migraine Prophylaxis — Is There an Evidence-Based Rationale? A Systematic Review.” Headache, 58:199–209 (2018). doi:10.1111/head.13217. Study design: Systematic review. n=5 RCTs.
- Cohen F, Bobker S. “From diet to disasters, lifestyle factors can affect headaches and migraine.” Headache, 63(6):712–713 (2023). doi:10.1111/head.14515. Study design: Editorial/Expert commentary.
- Khorsha F, Mirzababaei A, Togha M, Mirzaei K. “Association of drinking water and migraine headache severity.” Journal of Clinical Neuroscience, 77:81–84 (2020). doi:10.1016/j.jocn.2020.05.034. Study design: Cross-sectional. n=256.
- Spigt M, Weerkamp N, Troost J, van Schayck CP, Knottnerus JA. “A randomized trial on the effects of regular water intake in patients with recurrent headaches.” Family Practice, 29(4):370–375 (2012). doi:10.1093/fampra/cmr112. Study design: RCT. n=102.

